A Gastroenterologist’s review of what the evidence really says about the most prescribed laxatives for constipation
So you incorporated my dietary advice to improve constipation…
https://drhussenbux.substack.com/p/constipation-remedies
And you’re still constipated?!
Not to fear….you likely need some medication to help you…However…
Not all constipation medications are created equal.
While there are lots of options, only three of the five most commonly used treatments have robust scientific support. One popular medication is essentially ineffective, and another carries potential safety risks that you should be informed about.
This evidence-based review cuts through the noise to reveal what randomised controlled trials and the evidence actually shows. Let’s start!
Important disclaimer: If you are experiencing persistent constipation despite dietary modifications, seek specialist evaluation before self-treating. New or chronic constipation can signal underlying conditions including structural abnormalities, inflammatory disorders, metabolic conditions, or neurological issues that require proper diagnosis and targeted treatment. This guide reviews over-the-counter options for functional and established+simple constipation only.
1. Polyethylene Glycol (PEG): The Undisputed Champion
A systematic review of 10 randomised controlled trials found PEG increases stool frequency by 1.98 bowel movements per week compared to placebo. Head-to-head trials show it outperforms lactulose by 1.0-1.65 additional stools weekly while causing fewer side effects.
How PEG Works
Each PEG molecule binds up to a LOT of water molecules, creating an osmotic gradient that draws fluid into the intestines. Unlike stimulant laxatives, PEG isn’t absorbed by the body – it passes through unchanged, making it remarkably safe for long-term use.
Water retention softens stool and increases volume, triggering natural peristalsis without forcing contractions. This physiologic approach explains why 77-94% of patients achieve complete symptom resolution with continued use.
Clinical Evidence
The American Gastroenterological Association awards PEG its Grade A recommendation based on overwhelming evidence:
- Superior efficacy: 2.34 additional bowel movements per week in high-quality studies
- Rapid onset: Most patients see results within 2-4 days
- Sustained effectiveness: Six-month studies show no tolerance development
- Minimal side effects: Mild bloating in 18% of users, occasional loose stools
- Safety across ages: Proven effective from infants to elderly patients
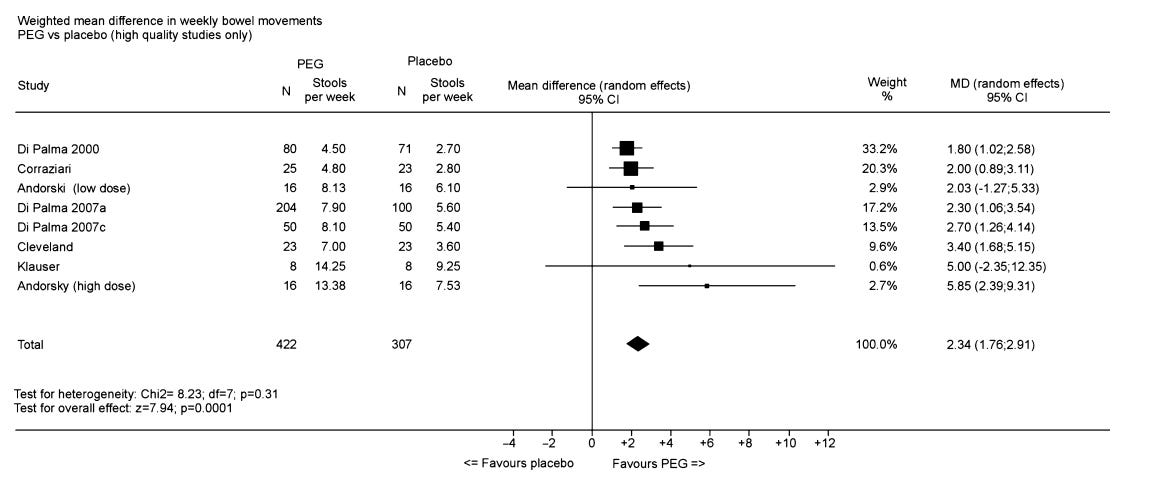
Weighted mean difference in weekly bowel movements PEG vs. placebo (high quality studies only
Who Benefits Most
PEG works for virtually everyone but proves especially valuable for:
- Chronic constipation sufferers requiring daily treatment
- Elderly patients sensitive to electrolyte disturbances
- Those taking constipating medications like opioids
- Patients with irritable bowel syndrome with constipation
PEG doesn’t require specific timing with meals or excessive water intake.
2. Psyllium Husk: The Only Fibre That Delivers
How it works: Imagine a tiny sponge that can absorb 50 times its weight in water. That’s essentially what psyllium does in your gut. When you mix it with liquid, it forms a gel that stays intact all the way through your digestive system, keeping your stool soft and bulky enough to trigger those natural muscle contractions that move waste along.
The evidence: A systematic review including 16 clinical trials with over 1,200 participants found that 66% of people taking psyllium experienced relief, compared to just 41% in control groups.
Your dose: Start with 5-10 grams daily (about 1-2 teaspoons) mixed in a full glass of water, and work up to 10-25 grams if needed. The key is consistency; most people see results after 4 weeks of daily use.
Pro tip: Always, always drink it immediately after mixing, and follow with another glass of water. This prevents it from gelling up in your throat (not dangerous, just unpleasant).

Senna earned its Grade A recommendation through consistent clinical success, joining PEG as the only over-the-counter laxatives with top-tier evidence ratings. This plant-based stimulant delivers predictable results but requires careful use.
A 2021 randomised controlled trial demonstrated among 90 patients with chronic constipation, 69% of senna users achieved treatment response versus 12% with placebo. The medication improved every measured outcome: spontaneous bowel movements, complete evacuations, and quality of life scores.
Mechanism and Timing
Senna contains anthraquinone compounds that activate intestinal nerves controlling muscle contractions. The cascade effect increases fluid secretion into the intestinal lumen, stimulates peristalsis throughout the colon, and accelerates transit time from 24-48 hours to just 6-12 hours.
This predictable timing makes senna ideal for planned relief. Taking senna at bedtime produces morning bowel movements in most patients.
Systematic reviews confirm senna’s effectiveness across populations. In elderly patients, it’s considered the “preferred agent regarding efficacy and safety.”
Join my newsletter….improving your liver and gut health…one e-mail at a time!
https://drhussenbux.substack.com/
Critical Limitations
Here’s where senna differs from PEG: time restrictions. Clinical guidelines limit recommended use to one week without medical supervision. The concerns include laxative dependence as prolonged use may impair natural bowel function, electrolyte losses from chronic diarrhoea that deplete potassium and sodium, melanosis coli which causes harmless but concerning dark pigmentation of the colon, and cathartic colon – a rare but serious loss of colonic muscle tone.
Side effects include cramping (common), diarrhoea (dose-related), and reddish-brown urine (harmless). Most patients tolerate short courses well.
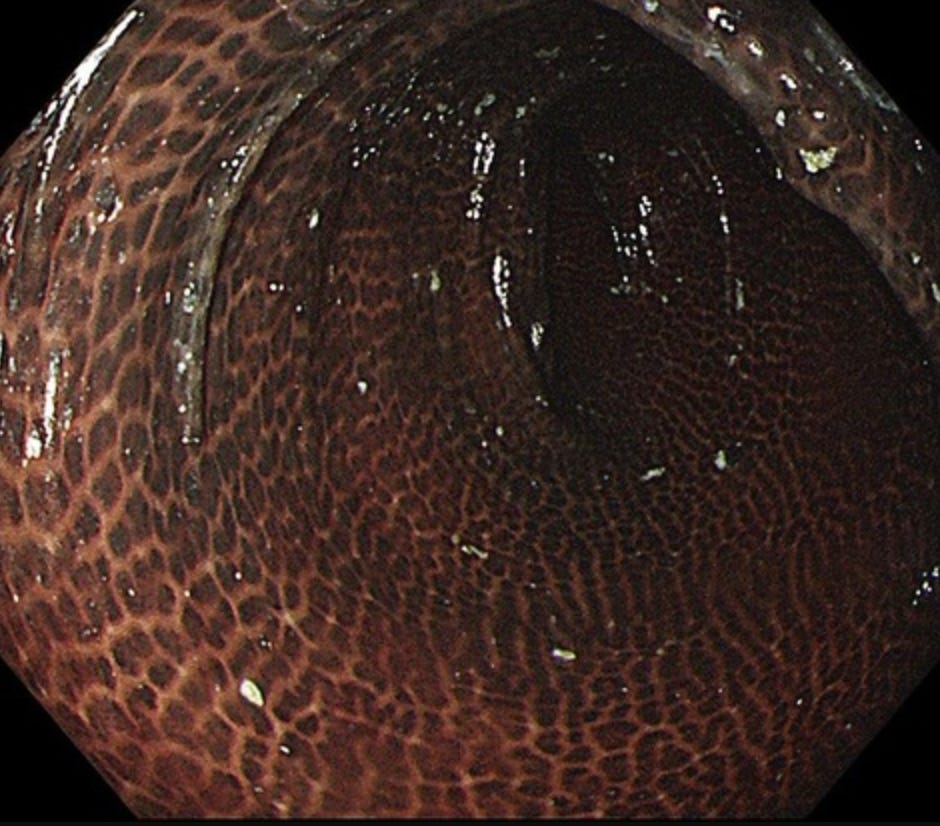
Too much senna and your colon looks like a leopard! Melanosis Coli
4. Docusate: The Emperor Has No Clothes
Prepare for a shock: docusate doesn’t work. Despite being one of the most prescribed laxatives worldwide, systematic reviews find no difference between docusate and placebo. The Journal of Hospital Medicine labeled docusate prescribing as something “we do for no reason.”
The Damning Evidence
Seven randomised placebo-controlled trials spanning 65 years reached the same conclusion: docusate fails to improve constipation. The numbers are stark. Stool frequency shows no difference from placebo, stool consistency sees no improvement, ease of passage provides no benefit, and patient satisfaction equals that of placebo.
A head-to-head trial delivered the knockout blow. While psyllium increased stool water content by 2.33%, docusate managed a pathetic 0.01% increase – statistically identical to doing nothing.
Why Docusate Persists
Explanations include historical momentum from being prescribed since 1955, a plausible mechanism as surface tension reduction sounds scientific, perceived safety with minimal side effects (because it does nothing), and ingrained clinician habits of reflexive prescribing patterns.
The American Gastroenterological Association diplomatically states that “properly designed RCTs are needed” – medical speak for “we can’t recommend this without evidence.”
The Path Forward
Progressive hospitals report 44% reductions in docusate prescribing after education initiatives. Patients switched to evidence-based alternatives like PEG or psyllium report dramatic improvements.
The message is clear: stop wasting time (and money) with docusate. Every day spent on ineffective treatment is a day of unnecessary suffering.

5. Phosphate Enemas: Fast but Furious
Phosphate enemas work within minutes however they should be seen as an SOS modality. You need to seek a specialist opinion before trialling this option.
Rapid Mechanism, Serious Risks
Phosphate enemas create an osmotic gradient that rapidly draws water from tissues into the colon. The dramatic fluid shift expands intestinal volume within 1-5 minutes, triggers urgent defecation through stretch receptors, and depletes body water and electrolytes.
There are studies that show increased morbidity, especially in elderly patients given phosphate enemas; therefore it should be used with caution.
The Safety Concerns
The FDA issued warnings about phosphate enemas after mounting adverse event reports. Electrolyte catastrophes include hyperphosphataemia (elevated phosphate), severe hypocalcaemia (depleted calcium), hypokalaemia (low potassium), and hypernatraemia (high sodium). These imbalances lead to clinical consequences including cardiac arrhythmias, seizures, acute kidney injury, tetany and muscle spasms, and in severe cases, death.
High-risk groups include anyone over 55 and patients with kidney disease, heart failure, or inflammatory bowel disease. Common medications like ACE inhibitors and NSAIDs increase risk.
When Enemas Make Sense
Despite the risks, certain situations warrant consideration, including faecal impaction unresponsive to oral treatment, pre-procedure preparation when oral prep fails, and neurogenic bowel in spinal cord injury patients.
The key: use saline enemas instead. Studies show equal effectiveness with dramatically lower risk. A randomised trial found enemas and high-dose oral PEG equally effective for impaction (80% vs 68% success).
Handle with care…
Making Evidence-Based Choices
The hierarchy of evidence points to clear treatment recommendations.
First-line treatment should be PEG, which offers the strongest evidence base, excellent safety profile, effectiveness for all ages, no tolerance issues, and cost-effectiveness.
Second-line options include psyllium, the only proven fiber supplement that provides additional health benefits as a natural option, though it requires proper technique.
For short-term use only, consider senna for rapid, predictable relief, but observe the one-week limit and monitor for dependence – it’s useful for acute situations.
Never use docusate as it’s no better than placebo and wastes time and money while providing a false sense of treatment.
Reserve phosphate enemas as a last resort due to serious safety concerns. Ideally use under hospital or specialist supervision.
P.S. What about lactulose? This osmotic laxative is the go-to treatment for hepatic encephalopathy (I will write a future newsletter on this topic), where it reduces ammonia absorption in patients with liver disease. For regular constipation, however, multiple trials show PEG outperforms lactulose with better efficacy and fewer side effects like bloating and flatulence
Ok so now you have the foods and the meds to treat your constipation
Decades of research provide clear answers about what works and what doesn’t.
PEG stands alone as the gold standard, offering unmatched efficacy and safety for chronic use.
Psyllium provides the only evidence-based fibre option, while senna fills a niche for short-term relief.
And docusate – a medication prescribed millions of times yearly based on tradition rather than evidence. Why use this when there are objectively better options out there?
Phosphate enemas remind us that “natural” doesn’t mean safe. Their rapid action comes with risks, therefore think of safer alternatives.
I now wish you all a regular once daily bowel motion!
Struggling with digestive issues that affect your daily life? Invest in your gut health with a private, personalised consultation where I will explore your specific symptoms and develop a targeted treatment plan. Take the first step toward digestive wellness today: https://bucksgastroenterology.co.uk/contact/
References
- Lee-Robichaud H, et al. Systematic review and meta-analysis: polyethylene glycol in adults with non-organic constipation. Int J Clin Pract. 2010;64(7):944-55.
- Attar A, et al. Comparison of a low dose polyethylene glycol electrolyte solution with lactulose for treatment of chronic constipation. Gut. 1999;44(2):226-30.
- Rao SS, et al. Efficacy and Safety of Over-the-Counter Therapies for Chronic Constipation: An Updated Systematic Review. Am J Gastroenterol. 2021;116(6):1156-1181.
- DiPalma JA, et al. A randomized, multicenter, placebo-controlled trial of polyethylene glycol laxative for chronic treatment of chronic constipation. Am J Gastroenterol. 2007;102(7):1436-41.
- Jalanka J, et al. The Effect of Fiber Supplementation on Chronic Constipation in Adults: An Updated Systematic Review and Meta-Analysis of Randomized Controlled Trials. Am J Clin Nutr. 2022;116(4):953-969.
- McRorie JW Jr. Evidence-Based Approach to Fiber Supplements and Clinically Meaningful Health Benefits, Part 2. Nutr Today. 2015;50(2):90-97.
- Giordano LA, et al. Psyllium is a natural nonfermented gel-forming fiber that is effective for weight loss: A comprehensive review and meta-analysis. J Am Assoc Nurse Pract. 2023;35(8):468-476.
- Belorio M, Gómez M. Psyllium: a useful functional ingredient in food systems. Crit Rev Food Sci Nutr. 2022;62(2):527-538.
- McRorie JW Jr, et al. Psyllium is superior to docusate sodium for treatment of chronic constipation. Aliment Pharmacol Ther. 1998;12(5):491-7.
- The role and therapeutic effectiveness of Plantago ovata husk (psyllium husk) in the prevention and non-pharmacological treatment of gastrointestinal diseases. Gastroenterol Rev. 2024;19(1):12-20.
- Senna Versus Magnesium Oxide for the Treatment of Chronic Constipation: A Randomized, Placebo-Controlled Trial. Am J Gastroenterol. 2021;116(1):152-161.
- Review of efficacy and safety of laxatives use in geriatrics. World J Gastrointest Pharmacol Ther. 2016;7(2):334-342.
- Petticrew M, et al. Systematic review of the effectiveness of laxatives in the elderly. Health Technol Assess. 1997;1(13):1-52.
- Fakheri RJ, Volpicelli FM. Things We Do for No Reason: Prescribing Docusate for Constipation in Hospitalized Adults. J Hosp Med. 2019;14(2):110-112.
- American Gastroenterological Association. AGA Clinical Practice Update on the Pharmacological Management of Irritable Bowel Syndrome With Constipation. Gastroenterology. 2023;164(1):146-151.
- Hasson BR, et al. Successful de-implementation of an ineffective practice: The fall of docusate. Am J Health Syst Pharm. 2023;80(23):1717-1724.
- Ladenhauf HN, et al. Toxicity of phosphate enemas – an updated review. Clin Toxicol (Phila). 2022;60(6):672-679.
- Ori Y, et al. Fatalities and severe metabolic disorders associated with the use of sodium phosphate enemas: a single center’s experience. Arch Intern Med. 2012;172(3):263-5.
- FDA Drug Safety Communication: FDA warns of possible harm from exceeding recommended dose of over-the-counter sodium phosphate products to treat constipation. FDA. 2014.
- Mendoza J, et al. Systematic review: the adverse effects of sodium phosphate enema. Aliment Pharmacol Ther. 2007;26(1):9-20.
General Disclaimer
Please note that the opinions expressed here are those of Dr Hussenbux and do not necessarily reflect the positions of Buckinghamhsire Healthcare NHS Trust. The advice is intended as general and should not be interpreted as personal clinical advice. If you have problems, please tell your healthcare professional, who will be able to help you.

